Welcome to Dr. Chadi Murr
Breast Reconstruction following a Breast Cancer – Plastic Surgery
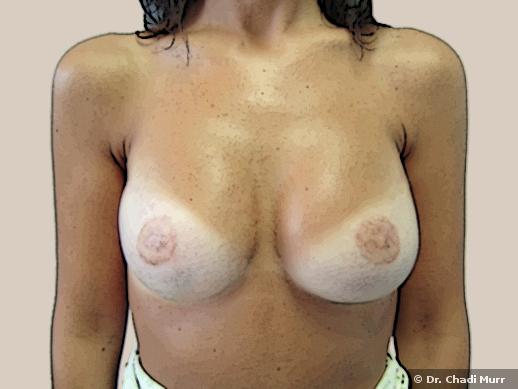
Breast reconstruction is a surgery performed on women who have undergone a mastectomy, which consists of removing breast tissue due to cancer. The aim is to provide the patient with two symmetrical breasts, even in size and shape.
Who should consider breast reconstruction?
Women who have only had lumpectomy, which is the partial removal breast tissue around the cancer removed, may not need reconstruction. Read More
However, patients who have had a mastectomy can consider breast reconstruction; it does not only change their physical appearance, but it also restores their sense of wellness and wholeness. The choice to have breast reconstruction is yours to make. You should discuss your concerns and ask about this type of surgery before you make your choice.
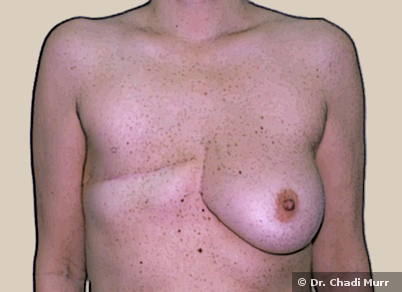
What are the different breast reconstruction options?
There are many techniques that can be performed in breast reconstruction: a newly shaped breast using implant, your own tissue flap, or a combination of both.
1- Reconstruction with implants
The silicone gel-filled implant is the most common one. Silicone gives a more natural-looking breast as its weight and texture are relatively similar to breast tissue. The surgery can be done either in one or two stages.
Read More
One-stage procedure: Immediate breast reconstruction can be performed at the same time with mastectomy. Once the general surgeon done with his part, I put a breast implant to replace the breast tissue to recreate the breast contour. Two-stage procedure: This reconstruction practice is done if the skin and chest wall tissues are tight and flat. A balloon-like tissue expander is put under the skin and chest muscles. A salt-water solution is then injected through a tiny valve at regular intervals to continuously fill the expander over a period of four to six months.
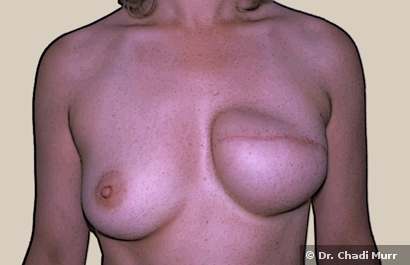
When the skin over the breast area is stretched enough, a second surgery is performed to replace the expander with the permanent implant.
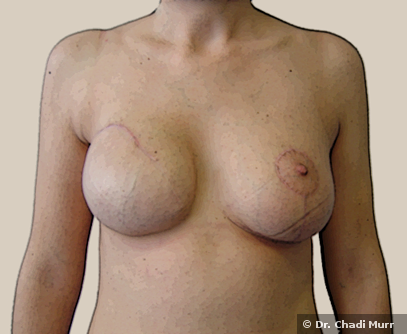
When during mastectomy the nipple and areola are removed, several techniques are available for nipple reconstruction; we can discuss the options according to the patient’s case.
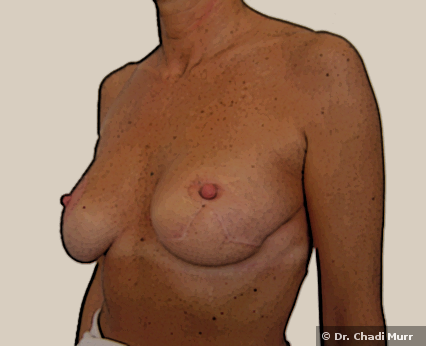
2- Reconstruction with tissue flaps
Also known as latissimus dorsi flap, this procedure consists of using tissues from the upper back to reconstruct the breast. Tissue flap surgery is also referred to as autologous tissue reconstruction.
Read MoreIn women with small breasts, the flap may supply sufficient volume and size without the use of implant. However, in women with larger breasts, it is necessary to include an implant at the time of the reconstruction. Careful preoperative markings are made and a flap consisting of the back muscle and its overlying skin and fat is elevated. A tunnel is then created under the skin, from the back to the new breast area. I will then move the flap, together with its blood supply, through the tunnel to the breast area.
This surgery is done with a single incision across the mid back area (hidden under the bra line). If an implant is to be used, it is placed underneath the flap on the chest wall. Since healthy blood vessels are needed for the tissue’s blood supply, flap procedures are usually avoided for women with diabetes, connective tissue or vascular disease, or for smokers.
How long is the recovery?
A recovery from an implant-based reconstruction is generally faster than one with flap, but both take two to three weeks of recovery.
Read MorePatients are usually sore after the surgery and experience pain when moving or lifting the arms. In some cases, flap-based reconstruction patients show weakness in their back, shoulder or arm after this surgery.
Patients can resume their normal lifestyle within four weeks; however, they should refrain from performing vigorous activities, such as running.
In all cases, you will be given specific instructions on how to care for your surgical site and what medications to take in order to relieve the pain and reduce the risk of infection. Be sure to ask all the questions concerning what to expect during the recovery period.
Disclaimer: The info presented on this page is indicative and for generic use only. Each patient’s case is unique and will be studied by Dr. Chadi Murr for full assessment.